Home » What Is Chikungunya? Transmission, Risks, and Cares

Chikungunya is a mosquito-borne viral infection that has emerged as a significant public health concern in many tropical and subtropical regions. Known for its sudden onset and intense joint pain, the chikungunya virus has impacted millions worldwide, particularly in areas where the Aedes aegypti and Aedes albopictus mosquitoes thrive. In recent years, increased travel, climate change, and urbanization have contributed to the spread of the disease into new territories, making awareness and prevention essential. In this article, we will explain everything you need to know about chikungunya virüs— from its causes and transmission to symptoms, risks, treatment, and prevention.
The chikungunya virus (CHIKV) is an alphavirus that belongs to the Togaviridae family. It was first identified during an outbreak in Tanzania in 1952. The name “chikungunya” comes from the Makonde language, meaning “that which bends up,” referring to the bent posture of patients due to severe joint pain.
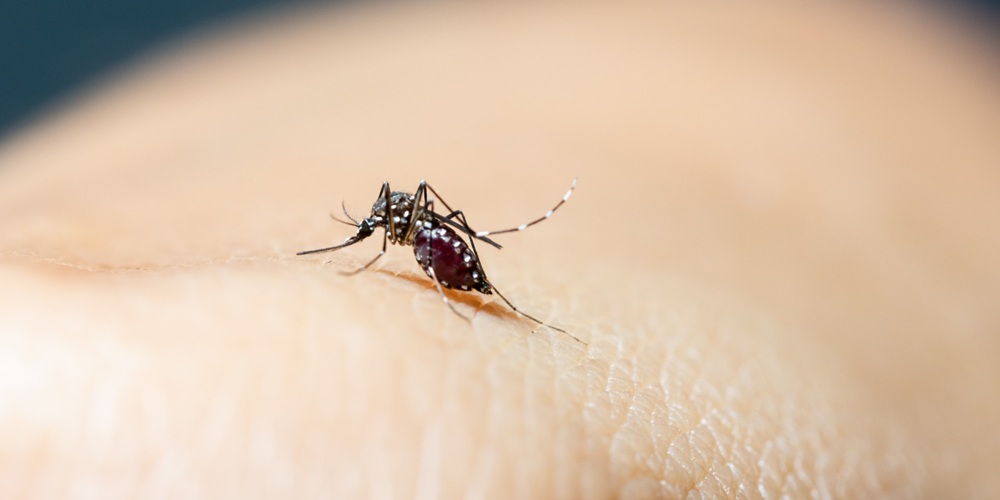
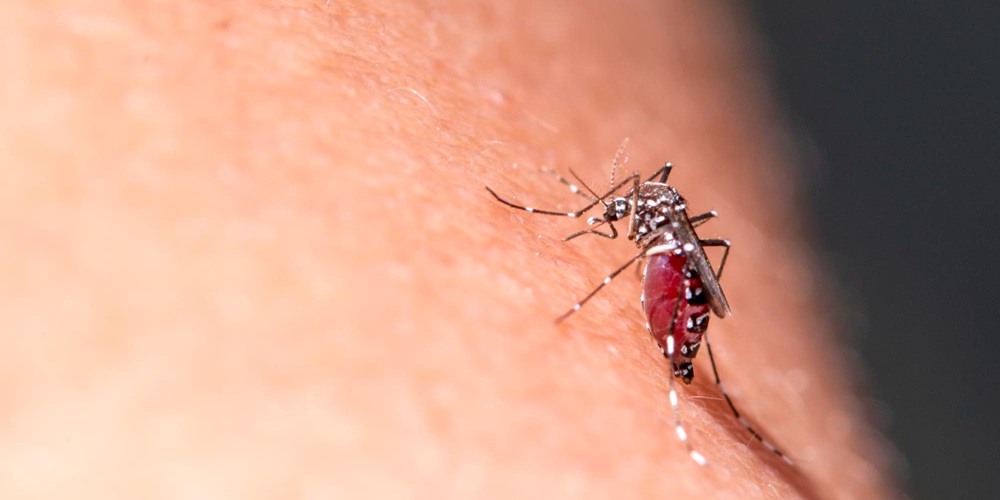
The virus is transmitted to humans through the bite of infected mosquitoes, primarily Aedes aegypti and Aedes albopictus, which are also known to spread dengue and Zika viruses.
The virus is transmitted to humans through the bite of infected mosquitoes, primarily Aedes aegypti and Aedes albopictus, which are also known to spread dengue and Zika viruses.
The cause of chikungunya is the chikungunya virus (CHIKV), transmitted to humans primarily through the bite of infected Aedes aegypti and Aedes albopictus mosquitoes.
Key points on chikungunya transmission:
Global travel, climate change, and inadequate mosquito control have significantly increased the spread of chikungunya in non-endemic regions.

Recognizing chikungunya symptoms early is essential for treatment and preventing further spread. Symptoms typically develop 2–7 days after infection and include:
While the fever may last only a few days, joint pain can persist for weeks or months, causing long-term discomfort.
Most patients recover completely, but chikungunya risks increase for vulnerable groups, such as:
Severe cases may lead to neurological disorders (encephalitis, meningitis), eye inflammation (uveitis, retinitis), and heart complications (myocarditis).

There is currently no specific antiviral drug for chikungunya treatment. Medical care focuses on:
Because no vaccine is commercially available yet, prevention is the most effective strategy.
Chikungunya prevention centers on mosquito control and personal protection:
Community-wide vector control programs are critical for reducing chikungunya transmission rates.
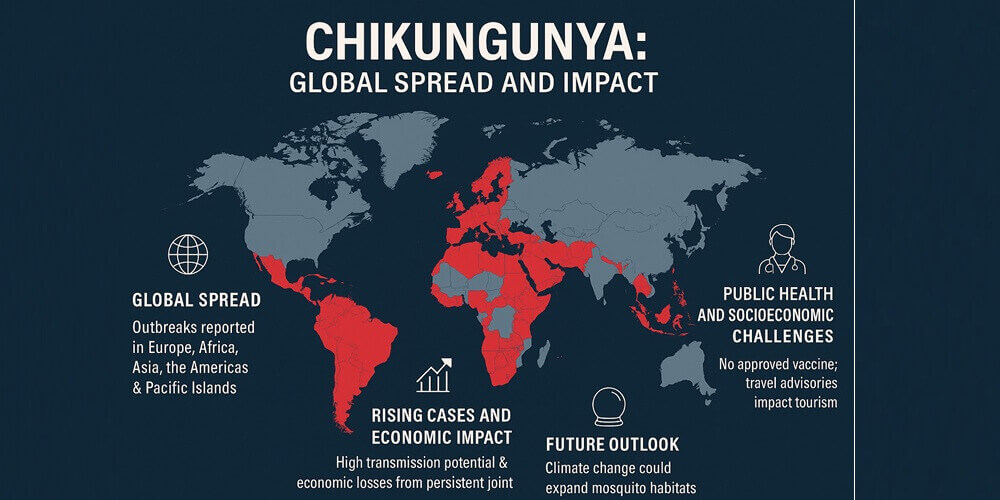
The global spread of chikungunya is linked to:
This means that even countries without a history of chikungunya outbreaks are now at risk.
While all three are mosquito-borne diseases, chikungunya virus differs in:
However, co-infections are possible, and proper medical testing is essential for accurate diagnosis.
Originally confined to tropical regions of Africa and Asia, the Chikungunya virus has expanded its reach over the past two decades. Since the mid-2000s, outbreaks have been reported in Europe, the Americas, and the Pacific Islands. Notably, the 2013 outbreak in the Caribbean quickly spread to South America, Central America, and even parts of North America. European countries like Italy, France, and Spain have also documented local transmission.
Experts warn that climate change could expand the habitats of Aedes aegypti and Aedes albopictus mosquitoes, enabling the Chikungunya virus to appear in regions where it has never been recorded before. The World Health Organization (WHO) recommends that countries strengthen vector control programs, improve public awareness, and implement early warning systems to prevent large-scale epidemics.
The increasing chikungunya risks worldwide highlight the need for strong public health education, effective mosquito control, and early diagnosis.
By knowing what causes chikungunya, how it spreads, and the best prevention strategies, communities can significantly reduce the number of cases.
Until an effective chikungunya vaccine is widely available, the best protection is vigilance, mosquito avoidance, and prompt medical care when symptoms arise.
https://www.who.int/news-room/fact-sheets/detail/chikungunya
https://my.clevelandclinic.org/health/diseases/25083-chikungunya
https://www.ecdc.europa.eu/en/chikungunya-monthly